All Departments
- Advanced Gait Evaluation & Management
- Ankylosing Spondylitis
- Cluster Headache
- Corticobasal Degeneration (CBD)
- Diagnostic Evaluation
- Disc Prolapse
- Dystonia
- Electrocardiogram (ECG)
- Electromyography (EMG)
- Epilepsy
- Guillain-Barré Syndrome (GBS)
- Headache & Pain Management
- Low Back Pain
- Low Back Pain
- Migraine
- Nerve Conduction Velocity (NCV)
- Neurological Disorder
- Other Chronic Headache Conditions
- Other Neurological Disorders
- Parkinson’s Disease
- Peripheral Neuropathy
- Personalized physiotherapy and mobility programs
- Potts Spine / Bone & Spine Tuberculosis
- Progressive Supranuclear Palsy (PSP)
- Radiculopathy
- Rehabilitation in various walking and movement disorders
- Rehabilitation Services
- Sacroiliitis
- Spasticity
- Specialized Treatments
- Spine & Musculoskeletal Disorders
- Tension-Type Headache
- Video EEG
Emergency Cases
+91 9839544407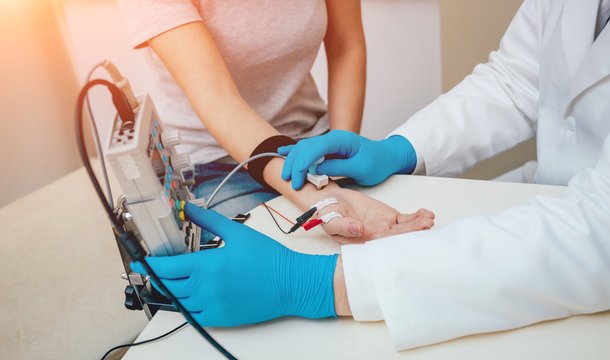
Electromyography (EMG)
Electromyography (EMG) is a specialized diagnostic procedure that measures the electrical activity produced by skeletal muscles. It is an essential test for evaluating muscle health and nerve function, often performed alongside Nerve Conduction Velocity (NCV) testing for a comprehensive neurophysiological assessment.
EMG is especially useful for diagnosing neuromuscular disorders, pinpointing the location of nerve or muscle dysfunction, and guiding effective treatment and rehabilitation plans.
Purpose of the EMG Test
EMG testing helps in diagnosing and differentiating between nerve disorders, muscle diseases, and disorders affecting the connection between nerves and muscles. It is particularly useful for:
Identifying nerve injuries or compression (such as carpal tunnel syndrome or radiculopathy)
Diagnosing muscle diseases (myopathies)
Detecting neuromuscular junction disorders (such as myasthenia gravis)
Assessing peripheral neuropathies (including diabetic neuropathy and Guillain-Barré Syndrome)
Evaluating motor neuron diseases (such as amyotrophic lateral sclerosis, ALS)
Determining the cause of muscle weakness, cramping, or unexplained pain
How the Test Works
EMG measures muscle electrical activity in response to nerve stimulation:
Electrode placement: A fine needle electrode is inserted into the muscle to record electrical activity.
Muscle activity measurement: Electrical signals are recorded while the muscle is at rest, during slight contraction, and during maximum contraction.
Data analysis: The recorded signals are analyzed for patterns indicating nerve or muscle disorders.
The test is generally performed under medical supervision, and while mild discomfort or slight muscle soreness may occur, it is safe and well-tolerated.
What EMG Can Reveal
EMG results help differentiate between:
Neuropathy: Damage to peripheral nerves
Myopathy: Muscle disease
Neuromuscular junction disorder: Abnormal communication between nerves and muscles
Motor neuron disease: Disorders affecting nerve cells that control muscles
These findings are critical for accurate diagnosis and targeted treatment planning.
Preparation for the Test
Wear loose-fitting clothing for easy access to the muscles being tested.
Avoid applying lotions or oils on the skin before the test.
Inform your doctor about any bleeding disorders, implanted devices, or medications affecting muscle or nerve function.
Relax during the test to ensure accurate recordings.
Combined NCV and EMG Testing
EMG is often combined with Nerve Conduction Velocity (NCV) testing to provide a complete picture of nerve and muscle health.
NCV measures how fast electrical impulses travel through nerves.
EMG records muscle electrical activity and response.
Together, they are powerful tools for diagnosing complex neuromuscular disorders.
Advantages of EMG Testing
Provides direct assessment of muscle and nerve function
Detects early nerve or muscle damage before significant symptoms appear
Differentiates between nerve and muscle causes of weakness or pain
Guides effective medical or surgical interventions
Monitors disease progression and recovery during rehabilitation
Conditions Commonly Evaluated with EMG
Radiculopathy (Cervical or Lumbar)
Peripheral Neuropathy
Carpal Tunnel Syndrome
Guillain-Barré Syndrome (GBS)
Myopathies (muscle disorders)
Motor Neuron Disease (e.g., ALS)
Neuromuscular junction disorders (e.g., myasthenia gravis)
Muscle injuries or trauma
Our EMG Testing Facilities
High-precision electromyography systems for accurate diagnosis
Experienced neurophysiologists ensuring safe and comfortable testing
Integration with NCV and other neurodiagnostic studies
Comfort-focused testing environment with patient safety as priority
Goals of EMG Testing
Our objectives are to:
Detect and localize nerve and muscle abnormalities accurately
Differentiate between nerve, muscle, or junction disorders
Guide personalized treatment and rehabilitation
Monitor response to treatment and disease progression
Improve overall patient quality of life
